How to make your walking workouts more effective
Interval and Nordic walking can help you get in better shape, while mindful walking can help you relax.
Walking for exercise has the advantage of requiring no particular skills or equipment aside from a comfortable, supportive pair of shoes. The disadvantage is that it can become tiresome after a while. Try reinvigorating your walking routine with these unique twists on this popular kind of exercise to break up your dullness.
Every step counts, some factors are more important than others. Adding short bursts of brisk walking to daily strolls can raise your heart rate and increase your cardiorespiratory fitness more than merely walking at a slower pace. Purchase a pair of Nordic poles and use them while walking to engage more muscles and burn more calories. You can also utilize walking to practice mindfulness, a mind-calming technique that can help you relax and relieve stress.
Here are some ideas for how and where you can try these tactics.
Walking in intervals
This routine is only for experienced walkers, not beginners, Interval walking involves alternating short spurts of quick walking with slower strides. Walk briskly for 15, 30, or 60 seconds after a five-minute warm-up. Then, for an equal period, slow down and recover at a normal rate (or you may want to double your recovery time). Begin with shorter intervals of quick walking and progressively increase the length of time as your stamina improves over the weeks and months. Alternatively, you can maintain the intervals and lengthen your entire workout time. Both a smartwatch and a watch with second-hand works in keeping track of time. Instead of using time, you might utilize landmarks to identify your intervals. Take a quick walk for one or two city blocks, between two telephone poles, or a quarter lap around a local track, for example.
Related topic: 16 SPORTS TO KEEP YOU FIT ALL SUMMER
This is an ongoing research
Is it possible to predict your longevity based on your current or previous menstrual cycle? A study published in The BMJ on Oct. 3, 2020, linked irregular or menstrual periods that are long (defined as 40 days or more) both in adolescence and adulthood to a higher risk of early death (before age 70) than those with normal or short menstrual cycles. The researchers discovered that the link was stronger for fatalities from heart and blood vessel disease and among women who smoked, based on data from roughly 80,000 women who took part in the Nurses' Health Study II.
It's impossible not to observe a pattern when it comes to many prevalent chronic pain illnesses, such as fibromyalgia, migraine headaches, arthritis, or lupus. The majority of patients diagnosed with these diseases are women. Women are not only disproportionately impacted by diseases that cause chronic pain, but they also have a harder time acquiring a precise diagnosis and receiving adequate therapy.
Pain mystery.
It is unclear why women tend to be more likely to have pain problems that last longer than a short time. It may be due to genetics. A biological explanation for these discrepancies may exist. Tho, the onset of menstruation often causes migraines to worsen in females.
Post-traumatic stress disorder (PTSD) may also be triggered by trauma, including sexual assault, which might lead to additional symptoms such as chronic pain. Women are more likely to have post-traumatic stress disorder (PTSD) than males. Only ten per cent of women will be diagnosed with PTSD over their lives, whereas only four per cent of males will be diagnosed with the disorder.
What causes pain problems to be more prevalent in women?
Women tend to suffer more from pain problems than men, but far too many have to endure for longer than they should due to delayed diagnosis. One of the findings reported in a 2011 study done by the World Endometriosis Research Foundation showed that on average, a woman had to wait seven years from the time she first had symptoms to when she was diagnosed with endometriosis. Like the lining of the uterus, the tissue that causes endometriosis develops elsewhere in the body, resulting in inflammation and scarring.
Also often found in people with fibromyalgia is the delay in diagnosis. The condition is thought to originate in the brain's pain response region.
This is ongoing research.
Cancer treatment may be aided by gut microorganisms. This research is still ongoing and being watched.
Researchers at the National Cancer Institute's Center for Cancer Research discovered that changing the type of microbes in the gut helped people with metastatic melanoma (a type of skin cancer that is aggressive) react to immunotherapy treatments that had previously failed them.
This prevalent issue is frequently overlooked or misinterpreted. Pelvic organ prolapse, a disease in which the uterus, bladder, small intestine, or rectum bulges into the vaginal wall or drops down through the vagina, affects around half of the women over 50. However, unlike other prevalent health issues, many women are reluctant to discuss it, even with their doctors. Some people do it out of embarrassment, while others do it because they believe it's simply something they'll have to cope with as they get older.
Pelvic organ prolapse conditions
Normal positions of pelvic organs

Cystocele and urethrocele
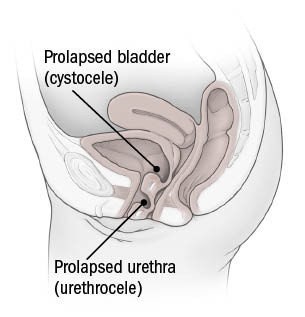
Rectocele

Uterine prolapse
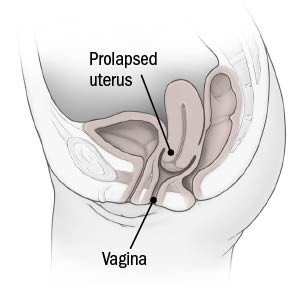
The topic of whether having the COVID-19 vaccination might impact my mammography findings was raised in an article authored by Kelly Bilodeau, Executive Editor, Harvard Women's Health Watch.
He explained that as your immune system prepares to detect and fight the virus, at least two of the authorized COVID-19 vaccinations may cause lymph nodes in the armpit (or other parts of the body) to swell. Although it's a safe transient response, it might cause some confusion on a mammogram. Swollen lymph nodes in the armpit or other surrounding areas are an indication of cancer in rare situations. Experts are now urging radiologists to use caution when interpreting the importance of enlarged lymph nodes observed on a woman's mammography if she has recently received the COVID-19 vaccination, to prevent unneeded testing and worry. If your breast imaging centre hasn't inquired about it, please do so. If your mammography reveals enlarged lymph nodes, your radiologist may recommend that you have further ultrasound testing or return in a few weeks to check if the swelling has subsided. If the swelling does not go away, further testing may be required. To minimize problems, schedule your mammogram before your first dosage or four to six weeks after your second dose. But don't forget to take the test and get your COVID-19 vaccine.
Browsing through venues is one of the most lust-worthy portions of the wedding planning process, right up there with engagement rings and bridal dresses. However, with so many options—at every price point— but it may be difficult especially if you aren't sure where you want to marry. Inspiration and direction are required even for the most imaginative bride.
Your wedding location, which is the most essential aspect of any wedding, makes the celebration spectacular. With years-long waitlists for the most sought-after destinations, it's important to prepare ahead, especially for the most awe-inspiration. Because the location you choose will appear in every image and memory from the day, it's critical to select a location that reflects the significance of the wedding, stunning all guests with its uniqueness.
Here are our top selections for the most beautiful wedding venues across the world, ranging from European chateaux to tropical beaches and unusual American locations.
Your baby has come after 40 weeks of doctor appointments, nursery preparation, and anticipation. You think she's wonderful, healthy, and cute. Over the next few weeks, your excitement is replaced with anxiety: Is she eating enough? Whoa, why does she cry? Is she ill? These concerns follow you around all day and night. You're right, irritated, and anxious. Your loved ones start to worry about you, not just the baby. You wonder if your stress is typical.
Baby blues, ptd, or pta? (postpartum depression, or postpartum anxiety).
You've probably heard of baby blues or postpartum depression. During your postpartum medical appointment, you may have been asked about your mood. Hormone levels drop after birth, causing feelings of sadness, weeping, and overwhelm. These symptoms are minor and only last a few weeks. It's possible that something else is causing the symptoms.
Symptoms of PPD and anxiety (such as poor sleep, trouble relaxing, and irritability). Some women have prenatal and postnatal anxiety, but only a small percentage of those parents experience postpartum depression. Postpartum depression can make it challenging for women to respond to treatments like interpersonal psychotherapy or prescription antidepressants like bupropion (Wellbutrin).
Momentary bouts of postpartum anxiety, like with postpartum depression, might be related to hormone fluctuations. It may also rise in reaction to actual pressures, such as the baby's health, money, or negotiating new responsibilities in relationships. If a woman has experienced pregnancy loss (miscarriage or stillbirth) this can enhance her chances of having postpartum anxiety. Anxiety symptoms may recur after birth if you had anxiety before or during pregnancy. Hormonal changes can cause anxiety and sadness after weaning.
Postpartum panic episodes or OCD symptoms are common. Fear, dread, panic, shortness of breath, and dizziness are among the signs of panic attacks. Unwanted thoughts and compulsions, or deliberate actions to ease discomfort, are called obsessions. Unsettling symptoms for new mothers, especially when they entail hurting the child. Fortunately, obsessions caused by anxiety disorders seldom cause harm to newborns.
Pin this post:
If you found this post enjoyable, kindly consider pinning it. Thank you, and may God bless you.




